|
As the fetus is only about 5-7 cm (the size of large shelled peanut), not every problem can be seen. The test has two parts. First, an ultrasound is performed which may be across the abdomen or across the vagina, or both, depending on the position of the fetus. The fetus is measured to make sure it is the right size and examined with the ultrasound. We check to make sure everything looks like it is developing normally. If your fetus is too big or too small, the test cannot be performed and will have to be rescheduled, so timing is very important. It is more likely to be covered if you are >35 years old, have an abnormality in your fetus or if you miss one of the other screening tests. You should check with your insurance to see if this test is covered.įetal nuchal translucency screen is performed between 10 and 14 weeks of gestation. It is a screening test for Down syndrome (trisomy 21), Edward syndrome (trisomy 18) and Patau syndrome (trisomy 13). These 3 conditions are all associated with developmental delay, and sometimes malformations in the newborn, therefore many parents want to know if these problems exist as early as possible. 
Unfortunately, this test is not always covered by insurance because it is a new test. This test can also detect several syndromes that occur due to microdeletions such as DiGeorge syndrome or Cri-du-chat syndrome (accuracy here is difficult to determine). This test cannot detect all genetic defects. It does not replace or give you nearly as much information as CVS or amniocentesis. It can tell you the gender of your fetus, if you desire. The first screening test a woman may have in pregnancy is called NIPS or non-invasive prenatal screening. This blood test can be performed any time after 9-10 weeks of pregnancy. It is sometimes performed by your doctor in the office, so if you are not sure if you have had this test, you should ask your doctor. This blood test measures DNA from the fetus in the blood of the mother. There is no risk to your baby from having this test. It is very accurate (99%) for detecting Down syndrome (also called trisomy 21), Edward syndrome (trisomy 18) and Patau syndrome (trisomy 13). For example, about 30% of fetuses with Down syndrome have no structural defects making it very difficult to detect with ultrasound alone. This is why genetic screening is done. Genetic screening in pregnancy is called “screening” because these tests do not detect all cases of genetic abnormalities. However, screening tests have no risk for the fetus (they are blood tests of the mother). In many pregnant women, multiple different screening tests are performed in an effort to detect as many abnormalities as possible. Some fetuses with genetic defects also have structural malformations, but not all. Malformations or structural problems with the body of the fetus or The most common reason a pregnant woman will see a maternal-fetal medicine specialist in pregnancy is to check the developing baby for abnormalities prior to birth. Unfortunately, not all abnormalities can be detected, however, those that can be detected fall into 2 general groups:ġ. Centrifuge and aliquot serum into a plastic vial within 2 hours of collection.NIPS: Non-invasive Prenatal Screening or Cell-free DNA The ultrasound and blood draw must be completed within a gestational window of 10 weeks, 0 days and 13 weeks, 6 days, which corresponds to a crown-rump length range of 31 to 80 mm.Ģ. Complete the NT/CRL Data for First Trimester/Sequential Maternal Screening.ġ. See Maternal Screening: Sonographer Approval Process. Do not send specimen to Mayo Clinic Laboratories if the sonographer is not NT-certified or before completing the application process. Nuchal translucency (NT) measurements are only accepted from NT-certified sonographers. Sequential maternal screening is a 2-part test that includes a first-trimester sample (this test) and a second-trimester sample (SEQB / Sequential Maternal Screening, Part 2, Serum).Īpproval to send specimen for first-trimester screening is required and may take up to 5 business days to complete. If a stand-alone neural tube defect risk assessment is desired, order MAFP1 / Alpha-Fetoprotein (AFP), Single Marker Screen, Maternal, Serum. If collecting a second-trimester specimen is expected to be difficult, order first-trimester screening instead (1STT1 / First Trimester Maternal Screen, Serum). 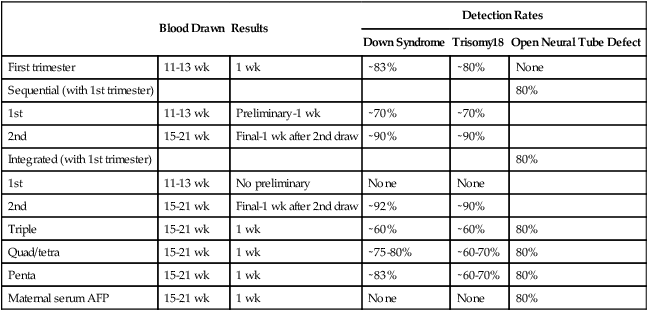 
When part 1 is negative, part 2 must be completed in order to receive an interpretable result.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
